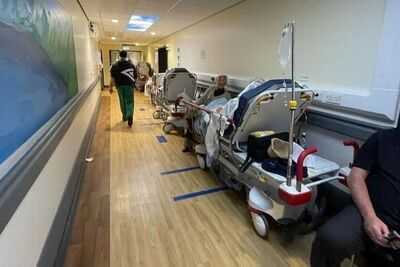
Nurses and doctors are too embarrassed to make eye contact with patients because of the hospital corridor care crisis, MPs have been told.
NHS staff leaders warned poor care having to be delivered in corridors and other spaces like store cupboards was a “national scandal” and is causing thousands of deaths. Corridor care was the subject of the Health and Social Care Committee on Wednesday morning. It comes after corridors have gone from becoming makeshift to permanent ward spaces with patients waiting many hours on trolleys to be admitted.
Dr Ian Higginson, president of the Royal College of Emergency Medicine (RCEM), said: “Corridor care is a visible symptom of overcrowding, which is a national crisis and, I believe, a national scandal. It's caused predominantly by long waits for admission to hospital.
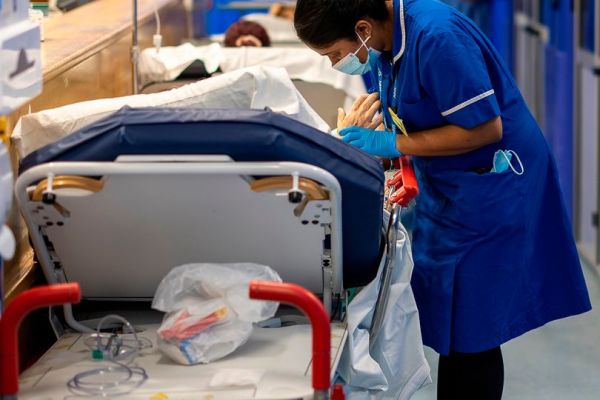
• Wes Streeting announces Labour will ‘end corridor care’ in NHS hospitals by 2029
• Labour makes biggest reduction in NHS waiting list for 15 years
“There is absolutely no safe or acceptable way to provide care for patients in corridors… it just cannot be done. We cannot understand why this hasn't got the focus it deserves because it's actively killing patients.”
NHS data shows patients who spent more than 12 hours in A&E are more than twice as likely to die within 30 days than those who are seen within two hours. More than half of Emergency Department Clinical Leads in England who responded to a survey published today by the RCEM said their A&E was unsafe for patients.
Dr Higginson said: “The conservative estimate is that some 16,000 patients a year are dying associated with long waits in emergency departments. That's a lot of patients. If this was any other sector there would be howls of rage. If it was an airline, we would be grounding aircraft. Yet this has been happening progressively worse year on year.”
The most elderly are more likely to have to endure the longest waits. It follows reports in a Royal College of Nursing (RCN) report in 2024 of patients dying “under a pile of coats” and in similar circumstances in packed waiting rooms.
RCN general secretary Professor Nicola Ranger said: “Nurses are often the ones closest to the patient. For many of them, that's what they feel very ashamed about as well, when they know that someone is stuck on a nurse's station and they need the toilet, or they're dying and they need a quiet space.
“I was talking to a patient there last week who said, it's that [nurses] feel embarrassed. So there's a lack of eye contact now. That is a symptom of people just, you know, head down because they feel upset with what they're seeing. And when their patients are struggling for a nurse to give them eye contact, that's not a good place.”
Dr Higginson, who also works as a consultant in an A&E, said: “I can say on a personal level that the phenomenon of avoiding eye contact is something I have experienced. For example, the waiting room announcement, I'm often asked to do it in my department. Many of the staff find it very difficult to simply go out into the waiting room and face the patients who've been waiting there for so long and explain what's been going on.”
A&E waits got steadily longer during over a decade of Conservative governments, before which waits over 12 hours were unheard of. By December 2019 some 2,356 patients waited longer than 12 hours on a trolley until a proper bed became available and by December 2025 it was 50,775 patients. Labour and NHS England have set an interim target of March 2026 for 78% of patients attending A&E to be admitted, discharged or transferred within four hours. Latest data shows 73.8% of patients in England were seen within four hours in A&Es.
Dr Rosie Bennyworth, chief executive of the Health Services Safety Investigation Board, told MPs: “We found corridors, sometimes store cupboards, kitchens and all sorts of areas being used for patient care that were not designed for this use.”
The NHS last month announced a change to how A&Es operate in an attempt to tackle the crisis. Emergency departments in England will open up dedicated areas for people who are likely to need "extended" care. NHS documents outlined a plan to prioritise patients with the most urgent need while avoiding "overcrowding". The change is aimed at making long waiting in emergency departments more bearable - particularly for the elderly for whom delays significantly increase the risk of death.
Older patients often live with multiple, complex health conditions so can take longer to diagnose. Patients will be identified to be safely monitored in extended emergency medicine ambulatory care areas (EEMACs) who are likely to be in A&E for between four and eight hours.
The blueprint outlines how a "model emergency department" should work and was aimed at helping thousands of patients to get faster emergency care. Medics are now supposed to be triaging patients upon arrival in A&E and can redirect them to other same-day clinics if they are more likely to get seen quicker and treated appropriately there.
Contact to : xlf550402@gmail.com
Copyright © boyuanhulian 2020 - 2023. All Right Reserved.